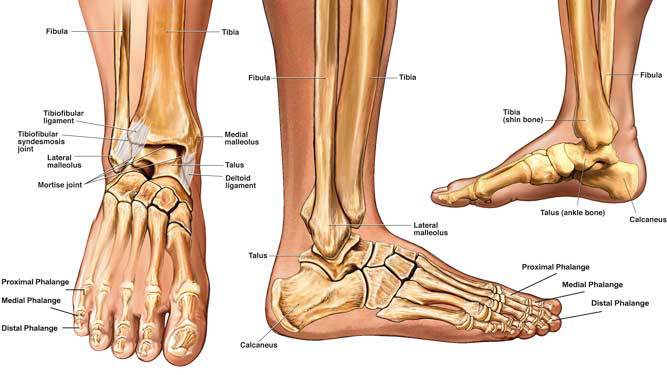
What is Metatarsalgia?
Metatarsalgia is a medical term used to describe pain that occurs in the ball of the foot. This occurs due to rubbing of the long bones of the foot, called metatarsals, causing inflammation. Build-up of inflammation in the ball of the foot compresses the small nerves that run between the toes and along the foot. Inflammation and compression of these small nerves is painful.
The pain can involve one or more joints of the foot including the big toe, second toe and third toe. It is unlikely to include the fourth or fifth joints. On occasion, the pain may involve the entire foot, or larger parts of the foot.
The pain or symptoms may be made worse when bearing weight through the foot, such as walking or running. In severe cases, just standing or even wearing tight footwear can affect the foot.
How does it happen?
Metatarsalgia can be caused by a number of things. An abrupt change in posturing of the lower back or pelvis may alter the way the foot is loaded, and cause rubbing of the long bones. Altered loading of the foot may also be caused arthritic conditions that affect the knees, hips or pelvis and carrying extra weight.
Unavoidable factors, which may lead to the development of metatarsalgia, include increased age, and the physical shape of the foot and toe. As your body ages, the ligaments of the foot may loosen or weaken. Therefore, the bones of the foot move differently leading to altered positioning and loading of the foot.
Avoidable factors, which may lead to the development of metatarsalgia, include wearing inappropriately fitting footwear, and the type of exercise performed. Metatarsalgia is more highly associated with high impact-type exercise such as running or gymnastics.
What are the signs and symptoms of Metatarsalgia?
The signs and symptoms of metatarsalgia may vary from person to person. Generally, a complaint of pain is common. This may range from mild to severe, or may be described as burning or shooting pain in the foot or toes. Another common description is a tingling sensation in the foot or toes.
Typically, symptoms worsen when weight bearing and improve once weight is removed from the foot.
How can Physio help?
Your physio will determine the cause of the metatarsalgia pain and assist you with adapting your posture, or improving the loading pattern of your foot. You may be advised to unload the foot by reducing or stopping exercise, changing the shoe you wear, or strengthening certain muscles in your legs.
Electrotherapeutic modalities such as icing, ultrasound or interferential therapy may be of assistance to reduce pain and inflammation in the beginning stages of treatment as well.
Please click the download button below to print out a free copy of our newsletter.